
#AMNIOTIC FLUID INDEX FREE#
SDVP is a semi-quantitative method that measures the largest vertical pocket of amniotic fluid, free from fetal parts or loops of umbilical cord ( 14).
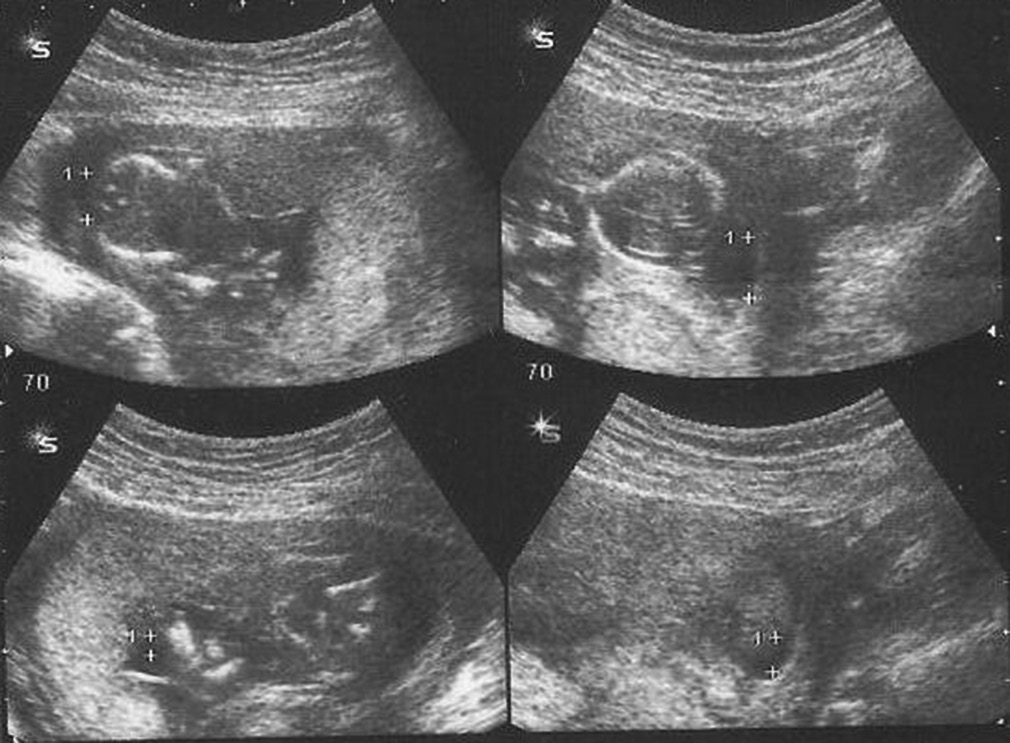
Amniotic fluid volume was determined for each patient at least 2 days before delivery, measuring both SDVP and AFI. All pregnancies were uncomplicated, without any maternal and/or fetal disease patients with fetal anomalies and/or abnormal fetal karyotype, detected during pregnancy or at delivery, were excluded. Gestational age was calculated from the date of the last menstrual period and confirmed at the first trimester scan. The mean maternal age was 33.1 ± 3.4 years (years ± SD range 24–45 years) and the gestational age at the time of the last ultrasound examination was 290.35 ± 1.42 days (days ± SD range 287–295 days). In the period between May 2011 and April 2013, we examined 961 singleton prolonged pregnancies at our Department.
At present, there is no consent about the efficacy in predicting adverse perinatal outcome with the ultrasonographic methods currently used to determine amniotic fluid volume ( 9– 13, 8).Īims of the present study concern: a) the comparison between the perinatal outcomes in prolonged pregnancies, complicated with oligohydramnios, and the outcomes in postterm pregnancies without oligohydramnios b) the evaluation of perinatal outcome in relation to different ultrasonographic methods for the examination of amniotic fluid volume in those cases complicated with oligohydramnios. In fact, oligohydramnios is usually associated with an increased risk of fetal heart rate tracing abnormalities, meconium-stained amniotic fluid and caesarean sections for fetal distress ( 6– 8). In this period of pregnancy, amniotic fluid volume is considered an important predicting factor of fetal wellbeing. It is probably related to a decrease in placental function and/or in fetal renal perfusion with reduction of urine production ( 3– 5). Frequently, postterm pregnancy is associated with oligohydramnios ( 2). Prolonged pregnancy is considered as menstrual age ranged from 41 to 41 6/7 weeks of gestation, while a pregnancy beyond 42 0/7 weeks is defined postterm ( 1). Middle cerebral artery Doppler velocimetry should be considered an investigational approach to antepartum fetal surveillance.Terms of postterm and prolonged pregnancy are poorly defined. If used in this setting, decisions regarding timing of delivery should be made using a combination of information from the Doppler ultrasonography and other tests of fetal well-being, along with careful monitoring of maternal status. Umbilical artery Doppler velocimetry seems to benefit only pregnancies complicated by intrauterine growth restriction. Recent, normal antepartum fetal test results should not preclude the use of intrapartum fetal monitoring. If repetitive late decelerations are observed, cesarean delivery generally is indicated. In the absence of obstetric contraindications, delivery of the fetus with an abnormal test result often may be attempted by induction of labor with continuous monitoring of the fetal heart rate and contractions. Oligohydramnios, defined as no ultrasonographically measurable vertical pocket of amniotic fluid greater than 2 cm or an amniotic fluid index of 5 cm or less, requires (depending on the degree of oligohydramnios, the gestational age and the maternal clinical condition) delivery, or close maternal or fetal surveillance. Subsequent management should then be predicated on the results of the contraction stress test or biophysical profile, the gestational age, the degree of oligohydramnios (if assessed) and the maternal condition.
#AMNIOTIC FLUID INDEX FULL#
Any significant deterioration in fetal activity requires fetal reevaluation, regardless of the amount of time that has elapsed since the last test.Īn abnormal nonstress test or modified biophysical profile usually should be further evaluated by a contraction stress test or a full biophysical profile. When the clinical condition that prompted testing persists, a reassuring test should be repeated weekly or, depending on the test used and the presence of certain high-risk conditions, twice weekly until delivery. In pregnancies with multiple or particularly worrisome high-risk conditions, testing may be initiated as early as 26 to 28 weeks of gestation. Initiation of testing at 32 to 34 weeks of gestation is appropriate for most pregnancies that are at increased risk of stillbirth. Women at high risk for stillbirth should undergo antepartum fetal surveillance using the nonstress test, contraction stress test, biophysical profile or modified biophysical profile.
